To her parent's surprise, her little sister was diagnosed with almost the exact same hearing loss two years later, also after being screened at the hospital where she was born. Both girls have been getting amazing support from the county Early Start Program since before they could sit up. And thanks, in large part, to early diagnosis and intensive interventions, they are both wonderful communicators!
 |
| http://blogs.rch.org.au/ccch/files/2011/08/BDP_2660.jpg |
National attention for newborn hearing evaluation peaked after the 1993 National Institutes of Health (NIH) Consensus Development Conference on Early Identification of Hearing Loss. This was a group of experts including otolaryngologists (aka Ears, Nose, & Throat doctors/ENT), speech and language therapists, audiologists, neurologists, speech pathologists, nurses, pediatricians, and more who came together to digest the science and make formal recommendations about why, when, how, and who to screen for childhood hearing loss.
What came of the Consensus conference were formal recommendations to implement 1) universal newborn hearing screening for all babies born in the U.S. 2) early intervention programs for those children identified as hard of hearing.
Hearing loss is actually one of the most common congenital birth defects, affecting 2 to 3 out of every 1,000 children. More than 50% of hearing loss is thought to be genetic.
At the time of the conference in 1993, the average age of diagnosis of hearing loss in children was three years of age. We know that language development literally starts as soon as a baby lands on this planet, and the most critical period of language and speech development is actually the first three years of life. Animal studies have shown that auditory deprivation during this time (i.e. not allowing animals to hear during the first years) actually interferes with the neuronal infrastructure, literally messing up the development of speech and language brain cells.
In other words, "You have to use it [your ears] or lose it [your hearing, speech and language]."
So, if congenital hearing loss wasn't being picked up until, on average age three years, and age zero-to-three is the most important period for speech and language brain development, we were missing a very serious window of opportunity to maximize a child's auditory potential. Especially because there are good studies that show that addressing hearing loss early does improve communication for the rest of that child's life.
Thank goodness, there has been remarkable progress.
Since 1993, all 50 states and the District of Colombia have established early hearing detection and intervention (EHDI) laws or voluntary compliance programs. Thirty-six states (including California) have legislated that hearing screens be performed at the time of birth in hospitals and birthing centers.
California's newborn hearing screen program started in 1998. Previously in California (and many other states) only "high risk" infants were being screened ("high risk" meaning babies who spent at least two days in the neonatal ICU-- these little guys actually have a 10-fold increased risk of being hard of hearing, those with structural skull or facial abnormalities, or those that had a family history of hearing loss). By screening only "high risk" babies, almost 50% of hearing loss was being missed at birth.
The National Center for Hearing Assessment and Management reports that detecting and treating hearing loss at birth for one child saves $400,000 in special education costs by the time that child graduates from high school.
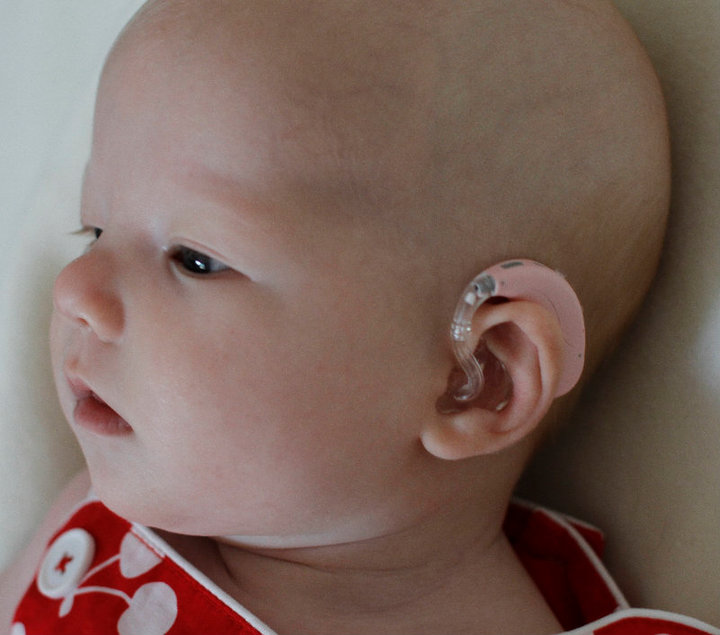 |
| http://www.speechbuddy.com/blog/wp-content/uploads/2012/07/Baby-with-Hearing-Aid.jpg |
Isn't that cool?! Not only does screening improve a child's quality of life, it actually saves the system money!
___________
How is the newborn hearing screen done?
There are actually two different ways to do a hearing screen:
1) Automated auditory brain stem response (ABR): the newborn's ears are covered with big headphones that emit a series of clicks. Electrodes placed on the baby's neck and forehead, measure brainwave responses to the clicks in the baby's brainstem. The computer compares those responses to "normal" responses and spits out a "pass" or "fail" report. See the video here.
2) Evoked otoacoustic emissions testing (EOAE) tests the cochlea, the part of the ear most involved in what is called peripheral auditory system. A small microphone is placed in the baby's ear canal and tests the cochlear ear cells echo response, also to clicks. Just like ABR, the computer generates a "pass" vs. "fail" report.
Both tests are relatively quick and easy and can be done within minutes on an alert but quiet newborn baby.
As I have mentioned in previous posts, there is almost always a downside to screening tests.The downside in the case of the newborn hearing screen is the potential for a large number of false positives. This means that many children who initially "fail" the screening test will actually wind up having normal hearing. Super stressful if you're a parent worried that your child might be hard of hearing. In fact, the rate of false positives is as high as 30% (i.e. 3 out of 10 "fails" will actually turn out to pass) if the test is done only one time; the number comes down to about 1% (1 in 10) if a "failed" test is repeated. So any time a baby doesn't pass initially, it's standard to repeat the screen as a double check. False positives can cause stress and anxiety for families during what is often already a stressful time; however, the risk associated with further evaluation is minimal (no invasive testing, no radiation), so I think it's probably worth it.
For those families who choose to have a birth center or home birth, the newborn hearing screen is still available to you through what are called "outpatient testing centers". Here is the link for all the California outpatient testing centers; those of you who live in other states should be able to ask your local hospital where the testing is available. It is covered by most insurances and Medicaid.
What happens if a baby does have hearing loss?
If a baby "fails" one of the screening tests, then the test is repeated. If the baby "fails" a second time, he/she is referred on for diagnostic testing and genetic evaluation. This has been shown to get the age of initiation of hearing aides down to about six months (Just as happened in the case of my friends' girls).
The goal of programs for early detection of hearing loss is to have a diagnosis in infants (before three months) and initiate services by six months of age. As happened for my friends, babies who don't pass the initial screen are referred onto diagnostic testing (Remember the difference between "screening" and "diagnosing": screening is meant to pick up anyone who MIGHT have the condition; diagnosis is meant to confirm of those picked up who ACTUALLY has it).
Babies who receive a diagnosis of hearing loss are referred to what in California is called the Early Start Program. But, don't fret, every state has a program for children ages 0-36 months who have a developmental delay and meet specific requirements. Check this site out for more information on the programs in your state.
Here is the important message: ANYONE can make a referral to Early Start, including parents, medical care providers, neighbors, family members, foster parents, and day care providers.
I was at the park just this week talking to a mother who was frustrated because she had broached the topic of her child's speech delay to her pediatrician, who then reassured her rather than referring her son for an evaluation. She continued to be convinced that her son needed some extra help and ultimately did the mama-bear thing and called herself. Please ask your primary care provider for guidance, but, seriously, if you don't feel like you are getting the help you need, trust your intuition. You can call yourself. The number for Early Start Services in California is (800)515-BABY.
What happened to my friends' little girls after they turned 3?
After our protagonists graduated from the Early Start Program at age three, these little ladies found themselves at the Jean Weingarten Peninsula Oral School for the Deaf (JWPOSD), a nurturing and rigorous environment that expanded on their early intervention and really got them ready to attend their local public school. Their mom told me, "JWPOSD not only taught the kids to listen and talk, but also to think." When the now-six-year-old's kindergarten teacher sent her mother a video of her sharing an "All about me" poster in front of 20 non-hearing-impaired classmates, her mom sent the video on to some of her former teachers and therapists. They were absolutely thrilled that the shy child they had taught was so expressive and confident. Success!
(On a random note, 70% of acquired hearing loss (i.e. hearing loss that wasn't present at birth but developed over time) is picked up by PARENTS. Please take note, providers, parental concern should be enough to merit evaluation. And parents, don't be afraid to speak up to your primary care provider!)
Additional references:
http://www.ncsl.org/issues-research/health/newborn-hearing-screening-state-laws.aspx
http://www.infanthearing.org/screening/index.html
http://www.aafp.org/afp/2007/0501/p1349.html
http://consensus.nih.gov/1993/1993HearingInfantsChildren092html.htm
http://www.asha.org/Advocacy/Issue-Briefs/
I was able to get rid of my herpes virus last year,i was diagnosed of herpes virus since late 2017 and i was on my doctor prescription ever since, I wasn’t satisfied i needed to get the virus out of my system,i was going through a blog to find new informations about the Herpes Simplex Virus i came across a review of a lady who was cured by (doctordohgo@gmail.com)I contacted the herbal foundation and they guided me on how to purchase the herbal formula.the herbal products las me for 3 weeks which helps me to get rid of the virus totally.
ReplyDeletewebsite ; doctordohgo.wixsite.com/herbs
whatsapp/call +2347062142293
I was diagnosed as HEPATITIS B carrier in 2013 with fibrosis of the
ReplyDeleteliver already present. I started on antiviral medications which
reduced the viral load initially. After a couple of years the virus
became resistant. I started on HEPATITIS B Herbal treatment from
ULTIMATE LIFE CLINIC (www.ultimatelifeclinic.com) in March, 2020. Their
treatment totally reversed the virus. I did another blood test after
the 6 months long treatment and tested negative to the virus. Amazing
treatment! This treatment is a breakthrough for all HBV carriers.